AI in healthcare isn’t a future promise anymore. It’s happening in operating rooms, radiology departments, drug labs, and on the wrists of millions of people tracking their heart rate every morning. The shift from “experimental technology” to “daily clinical tool” happened faster than most health systems were ready for. This transformation is part of a broader pattern where AI applications are reshaping how industries solve complex problems at scale.
In 2026, the conversation has moved on from “can AI help in medicine?” to “how do we govern it well, integrate it into workflows, and make sure it reaches everyone who needs it?” Here’s a look at the most important examples of that shift in action.
Smarter diagnosis with AI imaging
Medical imaging is where AI made its earliest and most dramatic impact, and it keeps getting stronger. Deep learning systems can scan X-rays, CT scans, and MRIs at a speed no human team can match, flagging subtle patterns that are easy to miss under the volume pressure most radiologists work under.
Google Health and DeepMind’s AI models for breast cancer detection have shown accuracy that rivals and sometimes exceeds specialist radiologists. Platforms like Aidoc and Rad AI process thousands of scans daily, sending real-time alerts to clinical teams when something urgent appears — a stroke, a pulmonary embolism, a fracture. These aren’t test environments anymore. They’re integrated into hospital workflows at major health systems across the US and Europe.
The National Institutes of Health has reported that AI systems demonstrate higher sensitivity in detecting conditions like lung cancer and diabetic retinopathy compared to traditional diagnostic methods. For radiologists facing hundreds of scans a day, having AI sort the urgent from the routine isn’t just a quality improvement — it’s a workload survival tool.
Predictive analytics and early detection
Predicting a health event before it becomes a crisis is one of the most valuable things medicine can do. AI is getting significantly better at it. Predictive models now analyze combinations of patient vitals, lab results, genetic data, and lifestyle patterns to identify risk long before symptoms appear.
In hospitals, real-time monitoring systems watch for subtle changes in a patient’s oxygen levels, heart rate, or blood pressure. When the pattern looks like early sepsis or cardiac deterioration, the system alerts the care team before the situation becomes acute. Companies like Health Catalyst build these platforms specifically for health systems dealing with high-volume inpatient care.
AI-supported precision medicine is now pushing this further. BCG research highlights that models tailored to individual genetics, environment, and lifestyle can potentially predict conditions like Alzheimer’s or kidney disease years before any symptoms appear. For patients with a family history of these conditions, that kind of early signal is genuinely life-changing. It turns a reactive system into a preventive one.
Personalized treatment and drug discovery
Precision medicine — the idea that treatment should be tailored to the individual rather than averaged across a population — has been a medical goal for decades. AI is finally making it operationally feasible.
Companies like Tempus and BenevolentAI analyze molecular data, patient records, and published research simultaneously to match patients with the therapies most likely to work for their specific genetic profile. BenevolentAI has active programs in rare diseases and inflammation where this approach is already producing clinical candidates at a pace that traditional methods couldn’t reach.
Drug discovery is where the timeline compression is most dramatic. Agentic AI — systems that can autonomously plan, generate, and simulate — is now being used to design new molecules and model how they’ll interact with biological targets. What used to take teams of chemists several years to screen and synthesize now takes months. That’s not a marginal improvement. It’s a structural change in how pharmaceuticals are developed.
A note on older tools: IBM Watson for Oncology, widely cited a few years ago for treatment recommendations, has been discontinued. Watson Health itself was sold and rebranded as Merative in 2022. The space has moved on to a new generation of purpose-built oncology AI platforms that are more tightly integrated with genomic data and real-world evidence.
Robotics and AI-assisted surgery
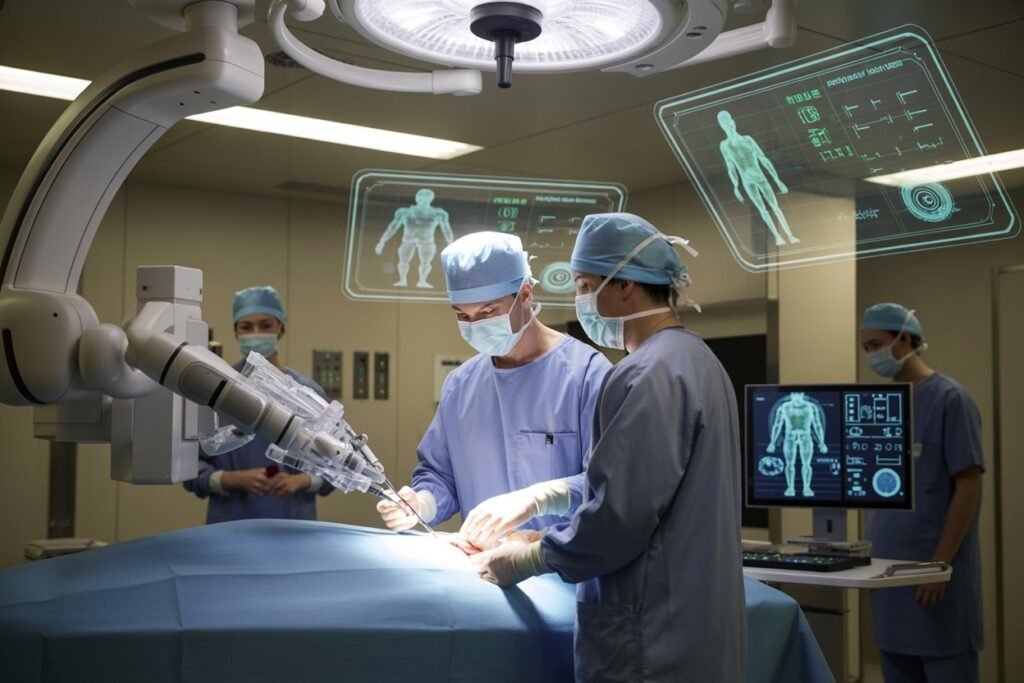
Surgical robots have been in operating rooms for years, but the AI layer on top of them keeps evolving. Systems like the da Vinci surgical platform and CMR Surgical’s Versius assist surgeons with delicate procedures where precision at the millimeter scale genuinely matters. The robot doesn’t operate independently — it translates the surgeon’s movements with greater stability and finer control than hands alone can achieve.
In orthopedic and neurosurgery, AI planning tools let surgeons model the procedure in 3D before making a single incision. The system maps anatomy, suggests optimal approach angles, and flags risks. Surgeons go into complex operations with more preparation than any previous generation had access to.
The post-surgery side is improving too. AI algorithms monitor recovery data and detect early signs of infection or complication before they escalate. Patients get personalized recovery plans that adjust based on how they’re actually progressing — not a generic protocol that fits no one perfectly.
AI co-pilots and the documentation problem
One of the most consistent complaints from doctors is time spent on paperwork instead of patients. AI is directly attacking that problem in 2026, and it’s one of the areas with the fastest real-world adoption.
Ambient AI scribes listen to clinical conversations and generate structured notes automatically. Microsoft’s Dragon Copilot is one of the most widely deployed examples — it transcribes and summarizes consultations, populating the patient record without the clinician having to type anything. Google has a similar suite of tools targeting administrative burden across health systems.
The results are meaningful. Clinicians report spending significantly more time in actual patient interaction when the documentation overhead drops. Health systems looking for efficiency gains without cutting staff see this as one of the clearest ROI cases for AI investment right now. The technology isn’t perfect — hallucinations in transcription are a real concern that researchers are actively working on — but for routine encounters, it’s already useful enough to be in daily use at major hospitals.
Beyond note-taking, AI handles scheduling, prior authorization requests, and patient follow-up reminders. These are the administrative tasks that eat hours out of a clinical team’s week. Automating them doesn’t replace anyone — it frees up time for the work only humans can do.
AI and mental health support
Mental health care has a chronic access problem. There are nowhere near enough therapists and psychiatrists to meet demand, and the waiting lists in most countries are long. AI isn’t solving that structural issue, but it’s creating real value at the edges of the system.
Digital support tools like Woebot and Wysa use conversational AI to deliver evidence-based exercises for anxiety and depression between therapy sessions, or as a first touchpoint for people who haven’t yet seen a professional. These tools don’t replace clinical care. But they reduce the gap between crisis and help.
More clinically, AI models trained on language data are showing promise in detecting early signs of mental distress through patterns in how people write and speak. Some platforms are being integrated into telemedicine systems to help therapists track patient progress between sessions and flag when someone may need more urgent attention. The technology is early but the direction is clear.
| How responsibilities split between AI and clinicians | |
| What AI handles well | What doctors still own |
| Scanning and flagging abnormalities in medical imaging at scale | Final diagnosis and clinical judgment within patient context |
| Monitoring vitals 24/7 and alerting on early warning signs | The conversation — empathy, trust, and the human side of care |
| Transcribing and summarizing clinical notes in real time | Ethical decisions, especially around end-of-life and risk tradeoffs |
| Screening millions of molecular compounds for drug candidates | Treatment decisions that involve patient values and preferences |
| Scheduling, admin workflows, and prior authorization processing | Accountability for outcomes — both legally and to the patient |
Data security, ethics, and the governance challenge
The more AI handles, the more data it touches — and healthcare data is among the most sensitive information that exists. This is where the conversation in 2026 has become genuinely serious.
“Shadow AI” — staff using unapproved AI tools outside official systems — surged through hospitals in 2025 as clinicians found their own ways to cut workload. The response in 2026 is a wave of formal governance frameworks: AI policy committees, approved tool lists, training programs, and audit systems. Health systems that got the implementation right are now focused on making sure the guardrails are in place for it.
On the technical side, approaches like federated learning allow AI models to train on patient data across multiple hospitals without that data ever leaving its source institution. This protects privacy while still allowing models to learn from large, diverse datasets. Regulations like GDPR in Europe and equivalent frameworks elsewhere set the minimum floor for how patient data can be used.
The deeper ethical question — how do you ensure an AI system doesn’t develop biases that produce worse outcomes for certain populations — is still being worked out. Healthcare AI that was trained predominantly on data from one demographic group can systematically underperform for others. This is now a recognized problem, and most serious AI health companies are actively working on it. But “working on it” and “solved” are not the same thing, and patients and clinicians deserve to know the difference.
What’s still standing in the way
The obstacles are real. Many smaller hospitals don’t have the cloud infrastructure that most AI tools require. Integration with legacy electronic health record systems is slow and expensive. Regulatory approval processes, while necessary, add time between a technology working in trials and being available in clinical practice.
There’s also the trust question. Doctors need to understand how a system reached its recommendation before they’ll act on it. “The AI said so” is not sufficient for clinical decision-making, and it shouldn’t be. The expectation in 2026 is that AI tools explain their reasoning clearly enough for a clinician to evaluate and challenge it.
None of this cancels out the progress. AI has the potential to give a rural clinic in an underserved region access to diagnostic tools that previously only existed in major urban hospitals. Remote monitoring, telemedicine, and AI-assisted diagnosis can make quality care available to people who currently have almost none. That’s the long-term case for this technology, and it’s compelling enough to justify working through all the hard parts. The same principle driving AI’s value here — technology serving people in the places they actually are — is what’s reshaping how cities move too, as autonomous systems make transportation safer and more accessible.